
Doctor of Medicine (MD) Program
Total Health Curriculum
The Total Health Curriculum is built on the science of learning and uses an evidence-based approach to train skilled, compassionate physicians who provide individualized care and promote health in the communities they serve.
Besides offering a fully integrated and immersive educational experience in basic, clinical and health systems sciences, the curriculum emphasizes six longitudinal themes:
- Social Justice and Health Equity
- Health System Citizenship
- Primary Care
- Personal and Professional Development
- Community Immersion
- Population Health
These themes are part of the Systems, Society and Humanism in Medicine (SSHM) core curriculum and will transform socially responsible students into socially accountable leaders in the healthcare system and their communities. SSHM develops compassionate and adaptable physicians dedicated to a person-centered approach to improving the health and well-being of the patients and communities they serve.
We liken our curriculum to a tree, similar to the tree of knowledge that forms our seal:
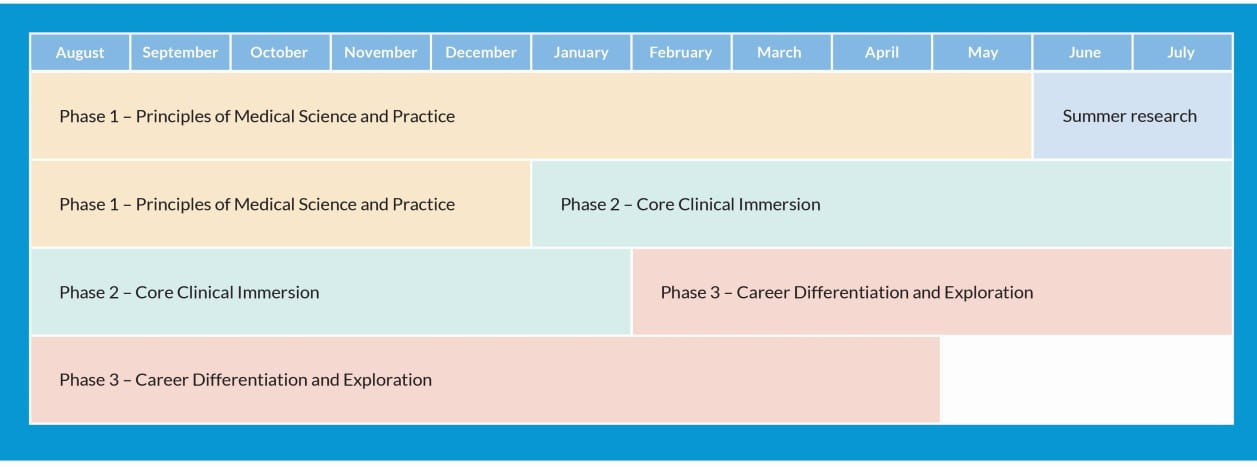
- Phase 1: Principles of Medical Science and Practice. This foundational education is rooted in basic, clinical and health system sciences.
- Phase 2: Core Clinical Immersion. The “trunk” is a solid body of clinical experiences that begins early and grows in complexity and meaning, providing firm support for the branches.
- Phase 3: Career Differentiation and Exploration. You’re now ready to branch off in your own direction. Following your core clinical experiences, you will progress in the development of advanced clinical skills and training that suits your individual interests and career goals.
At a glance: Total Health Curriculum
Why choose Geisinger Commonwealth School of Medicine?
Key features
- The science of learning: The Total Health Curriculum uses an evidence-based, active learning approach to medical education that has been demonstrated to improve learning. The curriculum is also grounded in principles of cognitive science and uses learning strategies including metacognition, spaced repetition, interleaving, retrieval practice and elaboration.
- The Clinical Presentation Model: The Total Health Curriculum relies on decades of educational evidence and ensures basic science and other content receive necessary emphasis in clinical context. This approach creates mental models to enhance learning, increases clinical relevance of early educational experiences and promotes recall during the clinical years and later in practice.
- Earlier clinical experiences: Students are placed in the primary care setting in their second semester as part of the Longitudinal Clinical Experience. Students are placed in their core clerkship rotations in January of their second year when they transition to Phase 2 of the curriculum.
- A team approach to teaching and learning: Clinicians and scientists work in interdisciplinary teams to create and implement the curriculum. This enhances the learning environment, provides clinical perspective and connects students early with Geisinger clinical faculty as role models and advisors for residency and specialty selection. Students also work in peer teams in class. These teams provide a supportive learning environment and help develop interpersonal skills necessary for medical practice.
- System-based learning. Geisinger Commonwealth immerses you into highly effective health systems for clinical learning experiences steeped in health systems science — all to prepare you to function in a 21st-century practice environment. We specialize in keeping patients healthy, as opposed to simply treating disease, which leads to better patient outcomes and a superior learning environment. You are an integral member of the healthcare team, in a role designed to maximize learning while benefiting patients.
- Research and scholarship: Numerous opportunities exist for you to investigate research opportunities in and outside of Geisinger and pursue supplemental funding to support your projects. Short- and long-term research programs include the Summer Research Immersion Program and the Medical Research Honors Program. You’re provided multiple opportunities to present research findings, including the annual Spring Research Symposium. You can also submit scholarly and creative work for publication in Geisinger Commonwealth’s journal for Scholarly Research in Progress (SCRIP).
- Career Pathway Program: This four-year required longitudinal curriculum embodies Geisinger Commonwealth’s mission and values. It lives within the Personal and Professional Development theme, integrated throughout our required courses. The program uses diverse instructional methodologies and includes a combination of self-assessments, interactive lectures, problem and case-based small group learning, panel discussions, residency application components, mock interviews, coaching and the e-portfolio. These activities support lifelong learning in the professional development process.
- Service learning: Service has always been integral to a Geisinger Commonwealth education. The Total Health Curriculum builds on this tradition by creating a more interconnected structure for immersion that collaboratively advances the work of our local service agencies. You’ll work with our community partners on projects that meet their needs to help provide solutions for their challenges. By being immersed in these experiences, you’ll understand community needs, how agencies work to meet these needs and how medicine can partner to deliver better health for individuals, families and entire neighborhoods — skills that will stay with you to improve communities anywhere.
